Mpox is a rare disease caused by infection with the mpox virus. The mpox virus is part of the same family of viruses as variola virus, the virus that causes smallpox.
About mpox
Currently there is a multi-national mpox outbreak with infections reported in all 50 U.S. states. In the current outbreak, hospitalization and death from mpox have been rare, but symptoms can be painful and affect daily activities.
Mpox in Idaho
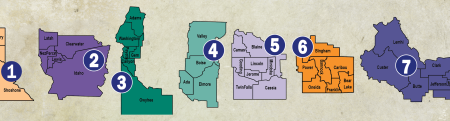
Local Public Health Districts

Mpox in the U.S.
Find an Mpox Vaccine Near You
What you should know about mpox
The most common symptom is a rash or sores that can look like pimples or blisters. These may be all over the body or just in certain parts, such as the face, hands or feet, as well as on or inside the mouth, genitals or anus. The rash and sores can be very itchy and painful, and sores in the anus or urethra can make it hard to go to the bathroom. Some people also have flu-like symptoms, such as sore throat, fever, swollen lymph nodes, headache, and tiredness.
If you develop a new or unexplained rash or other mpox symptoms, contact your healthcare provider.
Learn more about what to do if you are sick or have symptoms of mpox.
If you have symptoms of mpox, you should see a health care provider for testing. If you do not have a provider, contact your local public health district. Testing for mpox is available when ordered through healthcare providers.
Mpox can spread from person to person through direct contact with the infectious rash, scabs, or body fluids or by touching objects, fabrics (clothing, bedding, or towels), and surfaces that have been used by someone with mpox. It also can be spread by respiratory secretions during prolonged face-to-face contact or during intimate physical contact, such as kissing, cuddling, or sex.
Mpox can spread to others from the time symptoms start until the rash has fully healed and a fresh layer of skin has formed. Anyone in close personal contact with a person with mpox can get it and should take steps to protect themselves.
In the current outbreak, the majority of infections are occurring among gay, bisexual, and other men who have sex with men. However, anyone, regardless of sexual orientation or gender identity, who has contact with another individual with mpox is at risk. People more likely to get mpox may be eligible to receive a vaccine.
Other ways to prevent mpox include:
- Avoid close, skin-to-skin contact with people who have a rash that looks like mpox.
- Avoid contact with objects and materials that a person with mpox has used.
- Wash your hands often with soap and water or use an alcohol-based hand sanitizer, especially before eating or touching your face and after you use the bathroom.
Learn more about preventing mpox.
JYNNEOS vaccine is approved for prevention of smallpox and mpox for people 18 years of age or older when administered subcutaneously. It is authorized for the prevention of mpox when administred intradermally or subcutaneously among people 18 years of age and older and for use in people less than 18 years of age when administered subcutaneously. It is the primary vaccine being used in the U.S. during this outbreak.
The JYNNEOS vaccine is given as a two-dose series, 28 days apart. It is recommended to get the second dose on time, but it may be administered up to 35 days after the first dose. It is important to get both doses of JYNNEOS vaccine.
You are considered fully vaccinated against mpox 14 days after the second dose. Given the unknown effectiveness of vaccination in this outbreak, people who are vaccinated should continue to protect themselves from infection by avoiding close, skin-to-skin contact, including intimate contact, with someone who has mpox.
You should not get JYNNEOS vaccine if you had a severe allergic reaction after a previous dose of JYNNEOS. Talk to your healthcare provider if you have a history of an allergic reaction to the antibiotics gentamicin or ciprofloxacin or to chicken or egg protein.
Idaho has received a limited supply of vaccine doses from the federal government, and these have been distributed to local public health districts and some clinics. To find a vaccine near you, visit: https://mpoxvaxmap.org/
CDC recommends vaccine for people who have been exposed to mpox in the past 14 days. Vaccines may be offered to people more likely to be exposed to mpox, including:
Gay men and members of the bisexual, transgender, and gender non-conforming community who have had sex with men in the past two weeks and
- had multiple sexual partners or group sex,
- had sex at a commercial sex venue, or
- had sex at an event, venue, or in an area where mpox transmission is occurring.